Intramedullary Headless Compression Screws for Metacarpal and Phalangeal Fractures: A Surgical Guide
Introduction: A Revolutionary Fixation Approach
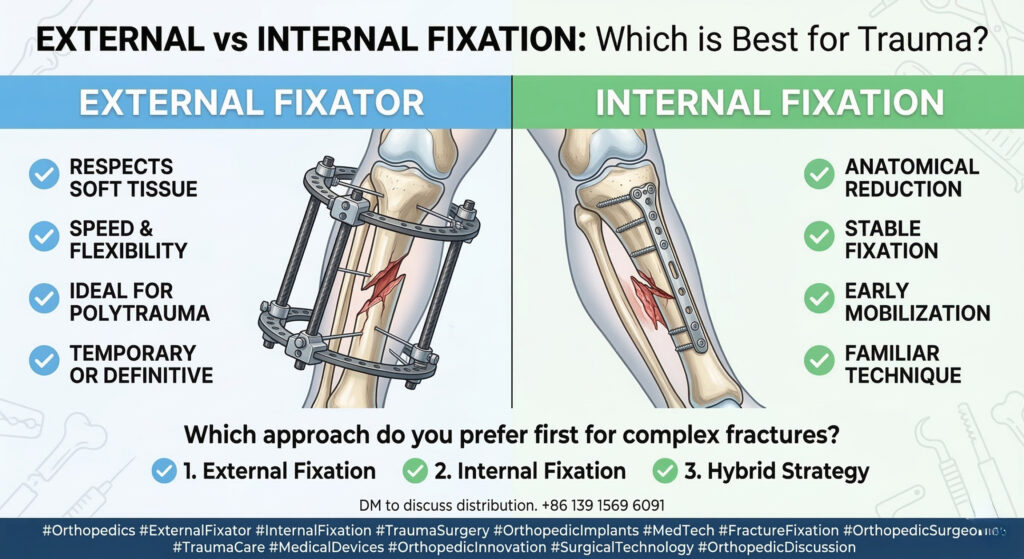
Metacarpal and phalangeal fractures are among the most common hand injuries, often resulting from trauma, falls, or sports-related accidents. Depending on the fracture type—simple transverse, comminuted, or open fractures—various fixation methods exist, including plate and screw fixation, percutaneous K-wire stabilization, or splinting. However, complications such as joint stiffness, flexion-extension limitations, and rotational deformities remain a challenge.
Enter intramedullary headless compression screws (IMCS)—a minimally invasive, biomechanically superior solution that promotes early mobilization and reduces soft tissue irritation. This technique is gaining traction in clinical practice due to its ability to maintain fracture stability while preserving soft tissue integrity.
In this guide, we analyze two key studies and provide a step-by-step breakdown of how IMCS fixation is applied to metacarpal and phalangeal fractures.
IMCS Fixation for Metacarpal Fractures
Indications for Use
IMCS is an excellent choice for:
✔ Transverse metacarpal shaft fractures
✔ Non-comminuted subcapital fractures
✔ Short oblique fractures
⚠ Preoperative Tip: Always measure the screw length and diameter accurately to ensure proper fixation.
Surgical Technique: Step-by-Step
Step 1: Closed Reduction
• Flex the metacarpophalangeal (MCP) joint to 90°.
• Make a 3.0mm longitudinal incision over the MCP joint.
Step 2: Guidewire Insertion
• Under fluoroscopy, insert a guidewire along the metacarpal axis.
• The entry point should be on the dorsal aspect of the metacarpal head, optimizing screw placement.
Step 3: IMCS Insertion
• Insert a 3.0mm headless compression screw into the metacarpal shaft.
• Ensure the threads fully bridge the fracture site to maximize compression.
👉 Pro Tip: Some studies recommend placing the screw up to the isthmus for optimal stabilization. Even in the fifth metacarpal, where a 5.0mm screw could fit, a 3.0mm screw is preferred to minimize cartilage damage.
Alternative: “Y” Configuration Fixation for Comminuted Fractures
For comminuted fractures, a single compression screw may compromise stability. Instead, use:
🔹 Two screws (3.0mm and 2.2mm) to create a triangular support structure.
🔹 This prevents collapse and enhances structural integrity.
IMCS Fixation for Proximal Phalanx Fractures
Technique 1: Intra-articular Approach
Surgical Steps
1. MCP Joint Incision: Make a 3.0mm incision at the MCP joint.
2. Guidewire Placement:
• Flex MCP to 70°, insert a guidewire dorsally under fluoroscopy.
• Dorsal subluxation of the phalanx may facilitate guidewire insertion.
3. Compression Screw Placement: Insert a 3.0mm or 2.2mm headless compression screw.
📌 Alternative: If joint subluxation is difficult, place the guidewire at a slight oblique angle without penetrating the joint.
Technique 2: Antegrade Intra-articular Fixation
When proximal phalanx subluxation is insufficient or the guidewire trajectory is unfavorable, use:
🔹 A 3.0mm incision at the MCP joint.
🔹 Flex the joint to 90° and insert the guidewire dorsally through the metacarpal head.
🔹 Advance the screw from the metacarpal head into the phalangeal base.
⚠ Drawback: This approach may damage the articular cartilage of the metacarpal head.
Technique 3: Retrograde Intra-articular Fixation
Alternatively, insert the IMCS in a retrograde manner:
✔ Make a 3.0mm incision at the proximal interphalangeal (PIP) joint.
✔ Flex PIP to 90°, insert a guidewire along the long axis of the phalanx.
✔ Advance the IMCS to the phalangeal base.
👉 While technically simpler, this method carries a higher risk of extensor tendon injury and cartilage damage.
Technique 4: Dual Antegrade Intra-articular Fixation
For comminuted fractures, single-screw fixation may be unstable. Instead, use:
🔹 Two antegrade IMCS to replicate the “Y” fixation method.
🔹 First screw: Insert at a shallow angle along the phalanx’s long axis.
🔹 Second screw: Place at a steeper angle for additional support.
⚠ Caution: Over-compression may lead to shortening of the phalanx—in such cases, a single-screw technique may be preferable.
IMCS Fixation for Middle Phalanx Fractures
Technique 1: Extra-articular Antegrade Fixation
• In transverse middle phalanx fractures, PIP joint subluxation may be challenging.
• Insert a guidewire obliquely from the ulnar base of the middle phalanx.
• Insert a 2.2mm IMCS for stable fixation.
Technique 2: Intra-articular Antegrade Fixation
If the guidewire trajectory is inadequate, use a PIP joint flexion to 90° approach.
✔ Insert a guidewire from the dorsal phalanx head to temporarily fix the PIP joint.
✔ Insert a 2.2mm IMCS into the middle phalanx.
Technique 3: Retrograde Intra-articular Fixation
Alternatively, insert a 2.2mm IMCS via the distal interphalangeal (DIP) joint.
⚠ Risks:
• Increased risk of extensor tendon damage.
• Higher probability of articular cartilage injury due to DIP joint’s small surface area.
Conclusion: Is IMCS Fixation the Best Option?
✔ IMCS provides a reliable alternative to K-wire and plate fixation, offering minimal soft tissue irritation and reduced joint stiffness.
✔ Indications: Best suited for transverse metacarpal fractures, non-comminuted subcapital fractures, and short oblique fractures.
✔ Limitations: Avoid use in open growth plates, infected fractures, or subchondral fractures.
✔ For comminuted fractures, dual-screw fixation (Y-configuration) prevents shortening and rotational instability.
📌 Clinical Pearl: IMCS is usually not removed unless protrusion, infection, or screw breakage occurs.
🔗 For further reading on IMCS techniques, check out this comprehensive study.
📢 Hashtags for SEO & Visibility:
#OrthopedicSurgery #HandFracture #IMCSFixation #MetacarpalFracture #PhalanxFracture #HeadlessCompressionScrew #SurgicalTechniques #HandTrauma #BoneFixation #MedTech