Pelvic Fracture Reduction Just Got Easier – Thanks to Surgical Robotics!
Displaced pelvic fractures have long been one of the most challenging injuries in trauma orthopedics. The complex anatomy, high risk of complications, and difficult reduction process make it a nightmare for surgeons. But what if there was a way to achieve precise fracture reduction with minimal invasiveness?
📢 Breaking News: A cutting-edge robot-assisted pelvic fracture reduction system has successfully performed its first surgery, proving its accuracy, safety, and effectiveness. Could this be the game-changer that trauma surgeons have been waiting for? Let’s dive in!
🔎 The Challenge: Why Are Displaced Pelvic Fractures So Hard to Fix?
Pelvic fractures are particularly difficult to manage due to:
• Complex anatomy – The pelvis is a critical structure housing major nerves, blood vessels, and organs.
• High risk of complications – Traditional open reduction internal fixation (ORIF) increases the chances of nerve damage, bleeding, and infections.
• Prolonged surgeries & radiation exposure – Surgeons often rely on fluoroscopy or CT guidance, leading to excessive radiation exposure and long surgical times.
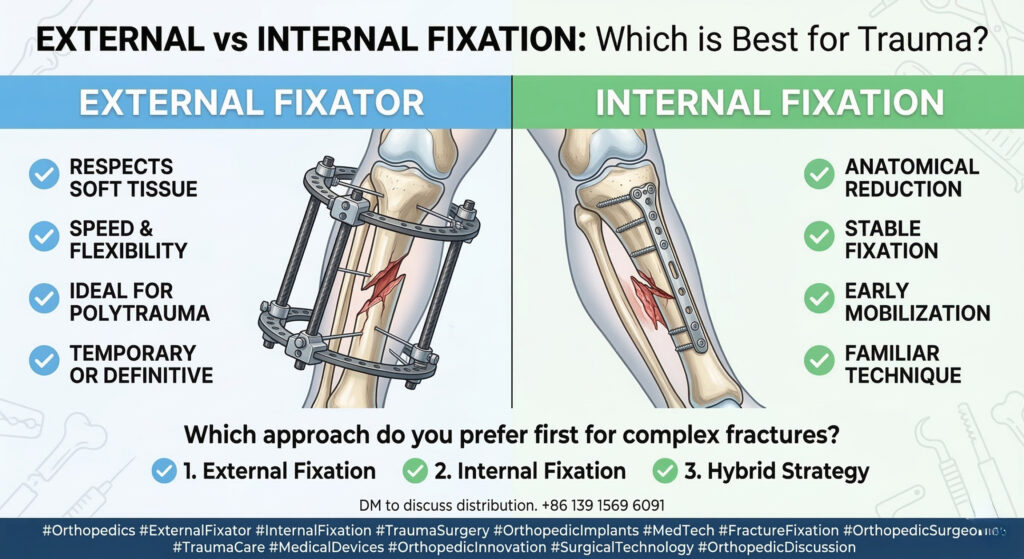
Traditional Approaches: ORIF vs. MIS
1️⃣ Open Reduction Internal Fixation (ORIF)
✔ Direct access to the fracture
❌ High complication rates – Increased risk of neurovascular injuries
❌ Long recovery times – Large incisions and extensive soft tissue damage
2️⃣ Minimally Invasive Surgery (MIS) with Percutaneous Fixation
✔ Less tissue damage, faster recovery
❌ Surgeon-dependent – Precision relies heavily on experience and intraoperative imaging
❌ Frequent fluoroscopy usage – Increased radiation risk
Despite advancements, robotic-assisted reduction remained an untapped area—until now!
🦾 Robotics in Pelvic Fracture Surgery: A True Game-Changer!
💡 What’s Different About This New Surgical Robot?
A next-generation robotic system has been designed specifically for autonomous fracture reduction. Unlike traditional techniques, this system can analyze fracture patterns, plan reduction paths, and execute movements with sub-millimeter accuracy.
Key Innovations of This Robotic System
✔ Pelvic Symmetry Reduction (PSR) Technology
• Uses AI-driven 3D modeling to create a mirror image of the healthy pelvis, guiding the fracture reduction process with unmatched accuracy.
✔ Elastic Traction Mechanism
• Unlike manual or rigid traction, this adaptive system applies continuous and stable force, optimizing the reduction while minimizing soft tissue damage.
✔ Autonomous Adjustment & Real-Time Monitoring
• The system self-corrects based on intraoperative imaging, reducing the need for excessive fluoroscopy and improving surgical efficiency.
👉 The result? A safer, faster, and more precise fracture reduction technique that outperforms traditional methods!
🏥 Clinical Breakthrough: A Real-World Success Story
A 56-year-old male patient sustained a Tile B2 unstable pelvic fracture due to a direct impact on the hip. Conventional reduction would have required a highly invasive procedure—but with robotic assistance, the surgery was completed with:
📌 Surgical time: 110 minutes
📌 Blood loss: Only 50 mL
📌 Post-op fracture displacement: ≤ 2.8 mm (Rated “Excellent” per Matta Criteria)
📌 Zero intraoperative complications
Recovery Timeline:
✔ Post-op Day 2 – Started range-of-motion exercises
✔ Week 2 – Partial weight-bearing allowed
✔ 3-Month Follow-Up – Full independent ambulation, Majeed functional score: 95/100 (“Excellent”)
📊 How Does Robotics Compare to Traditional Surgery?
| Method | Surgical Time | Blood Loss | Excellent Reduction Rate | Complication Rate |
|---|---|---|---|---|
| ORIF | ~152 min | ~250 mL | 75.8% | 7.5% |
| MIS (Conventional) | ~103 min | ~50 mL | 77.4% | Lower |
| MIS + Robotics (This Study) | 110 min | 50 mL | 100% | 0% |
🔥 Key Takeaway: Robotic-assisted fracture reduction delivers near-perfect alignment, fewer complications, and minimal soft tissue damage, making it a superior choice for pelvic trauma cases.
💡 What This Means for the Future of Trauma Surgery
✔ Increased Surgical Precision
Robotic real-time navigation and AI-powered adjustments improve accuracy and reduce the likelihood of malalignment.
✔ Lower Radiation Exposure
Fewer fluoroscopy scans mean less radiation risk for both patients and surgical teams.
✔ Shorter Recovery & Fewer Complications
Minimally invasive techniques combined with robotics ensure faster healing, less post-op pain, and lower infection risks.
🚀 Bottom Line: This revolutionary robotic system represents the future of pelvic fracture treatment, making surgeries safer, faster, and more efficient than ever before.
🌎 The Future Is Here: Will Robotics Become the Gold Standard?
With its unparalleled precision, lower complication rates, and improved patient outcomes, robotic-assisted surgery is poised to redefine trauma orthopedics. As technology advances, we may soon see these systems becoming a standard part of pelvic fracture management worldwide.
👉 What do you think? Will robotics replace traditional pelvic fracture surgery shortly? Share your thoughts in the comments! 👇
Disclaimer:
This article and all articles on this website are for reference only by medical professionals; specific medical problems should be treated promptly. To ensure “originality” and improve delivery efficiency, some articles on this website are AI-generated and machine-translated, which may be inappropriate or even wrong. Please refer to the original English text or leave a message if necessary. Copyright belongs to the original author. If your rights are violated, please contact the backstage to delete them. If you have any questions, please leave a message through the backstage, or leave a message below this article. Thank you!
Like and share, your hands will be left with the fragrance!