Understanding the language of orthopedics is fundamental for advancing expertise in the field. Whether you’re a surgeon, researcher, or student, mastering key terms enhances communication and comprehension of complex concepts. This glossary provides clear, concise definitions of essential orthopedic terminology, offering insights into procedures, materials, and pathologies. Dive into the world of orthopedic vocabulary and elevate your understanding today.
A – Foundational Orthopedic Terms
Allograft Bone
Definition: Sterile bone harvested from another human, used in grafting procedures.
Importance: Allografts are widely utilized in spinal fusion surgeries and other reconstructive procedures due to their ability to promote healing without requiring autografts from the patient.
Anterior
Definition: Refers to the front portion of the body.
Clinical Use: Terms like anterior cruciate ligament (ACL) highlight anatomical positioning critical in sports injuries and surgical planning.
Annulus Fibrosus
Definition: The fibrous outer ring of an intervertebral disc.
Significance: Damage to the annulus fibrosus often leads to conditions like disc herniation, requiring interventions such as discectomy.
B – Structural and Biologic Concepts
Bone Graft
Definition: Bone transplanted from one location to another, either from the same individual (autograft) or another donor (allograft).
Clinical Application: Bone grafts are critical in procedures like spinal fusion or fracture repair, ensuring structural stability and promoting osteogenesis.
Bioabsorbable Polymer
Definition: A material, such as certain plastics, that the body can naturally break down and absorb.
Use in Surgery: Bioabsorbable polymers are used in orthopedic implants, minimizing the need for removal surgeries.
Bone Plate
Definition: A thin metal device affixed to bone with screws to stabilize fractures.
Example: Bone plates are commonly used in comminuted fractures, where multiple fragments require immobilization for healing.
C – Cartilage and Cervical Spine
Cartilage
Definition: Hard, thin tissue covering the ends of bones at joints, enabling smooth motion with minimal friction.
Clinical Application: Damage to cartilage often results in osteoarthritis, a leading cause of joint pain and dysfunction.
Cervical
Definition: Refers to the neck region of the spine, comprising seven vertebrae.
Relevance: Cervical spine injuries, such as whiplash, are common in motor vehicle accidents and require precise diagnostic imaging.
D – Degeneration and Fixation
Disc Degeneration
Definition: Loss of structural and functional integrity in the intervertebral disc.
Impact: A leading cause of lower back pain, necessitating treatments like physical therapy or surgical interventions such as spinal fusion.
Distal
Definition: Situated away from the center of the body.
Example: Distal fractures, such as distal radius fractures, are among the most common orthopedic injuries.
E – Endoscopic Innovations
Endoscope
Definition: A medical device used to view internal structures, often equipped with fiber optics and video capabilities.
Application: Endoscopic techniques, like arthroscopy, allow minimally invasive joint surgeries with faster recovery times.
Excision
Definition: Surgical removal of tissue or material.
Clinical Use: Procedures like tumor excision or synovectomy rely on precise excision techniques to improve outcomes.
F – Fractures and Fusion
Comminuted Fracture
Definition: A fracture where the bone breaks into multiple pieces.
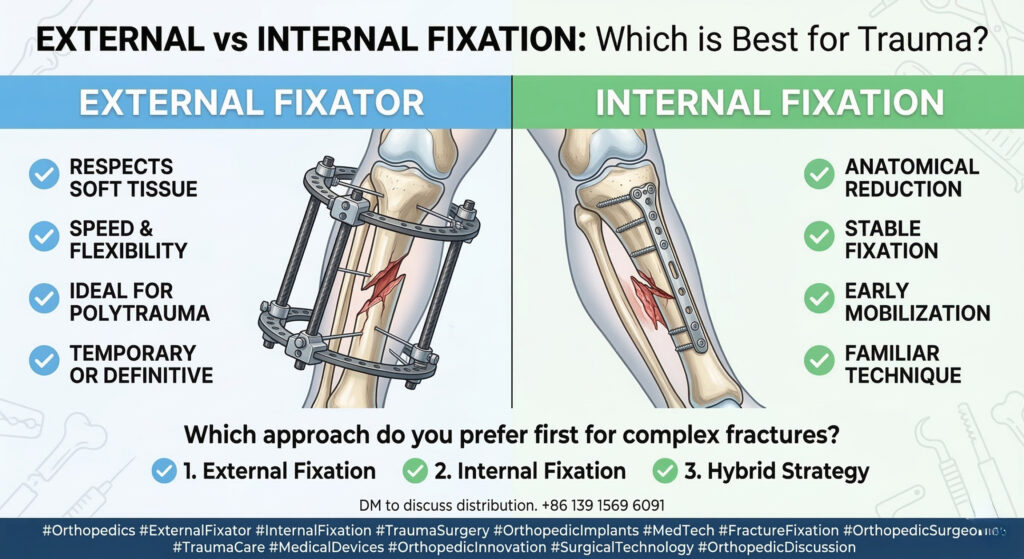
Treatment: Requires advanced fixation techniques, such as bone plates or external fixation devices, to ensure proper healing.
Fusion
Definition: The surgical union of bones, often across a joint space, to eliminate motion and promote stability.
Example: Spinal fusion is a cornerstone procedure for treating degenerative disc disease or scoliosis.