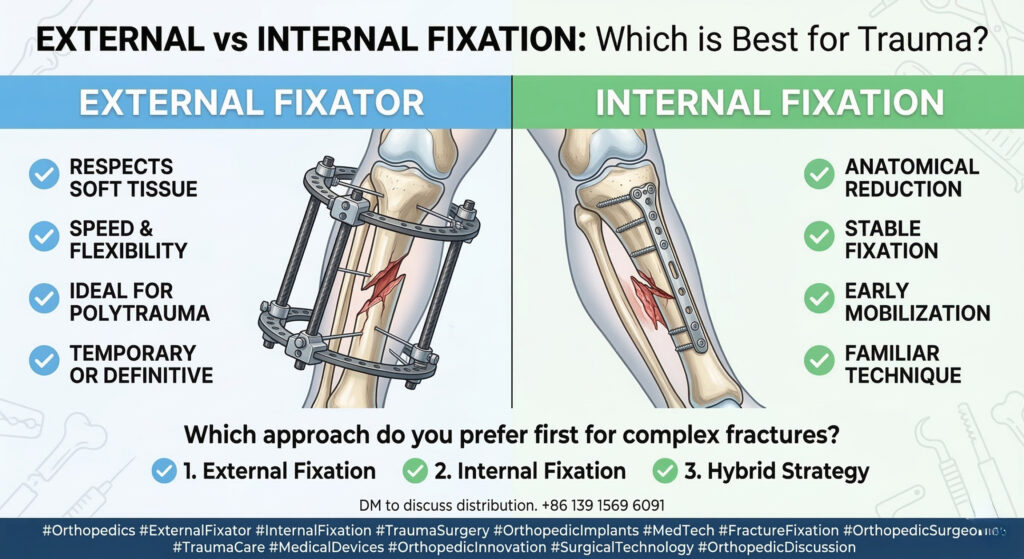
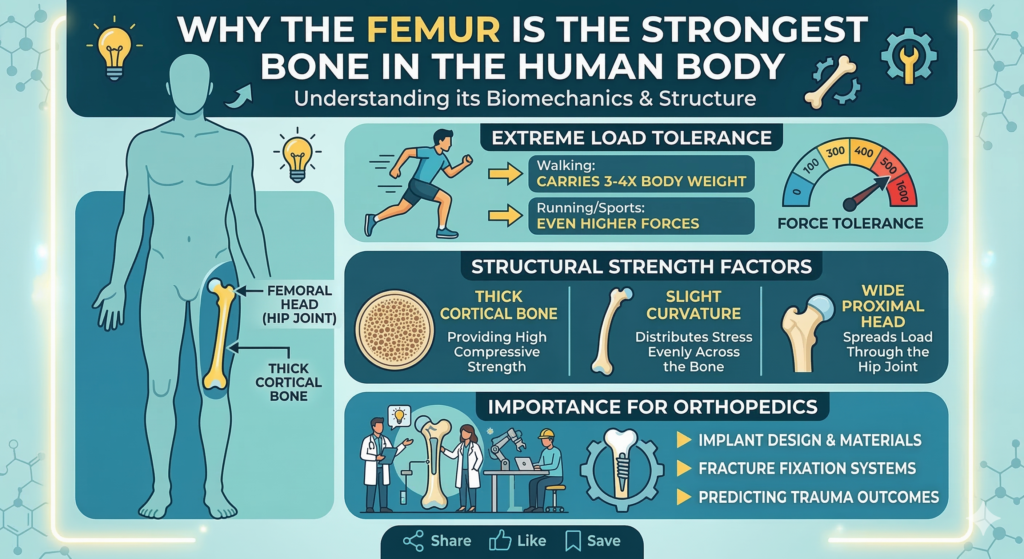
Pathogenesis: From “Synovial Herniation” to the One-Way Valve Mechanism
In the last decade, histopathology and imaging studies have reshaped our understanding of ganglion cysts. Forget the “synovial herniation” myth — the new Articular Theory prevails.
A ganglion cyst is a pseudocyst, with a dense collagen wall and no synovial lining. The content? Not synovial fluid, but viscous mucin, rich in hyaluronic acid and mucopolysaccharides.
The key mechanism:
- Trigger: Repetitive microtrauma or degeneration (commonly from the scapholunate ligament) causes mucinous degeneration of connective tissue.
- Formation: A capsular rent connects the joint space and the cyst.
- Maintenance: A one-way valve effect pumps joint fluid into the cyst, but prevents return — explaining its fluctuating size and frequent recurrence.
👉 In short: Ganglion cyst = mucinous degeneration + unidirectional joint communication.
This also explains why complete excision of the cyst stalk and joint capsule opening is key to long-term success.
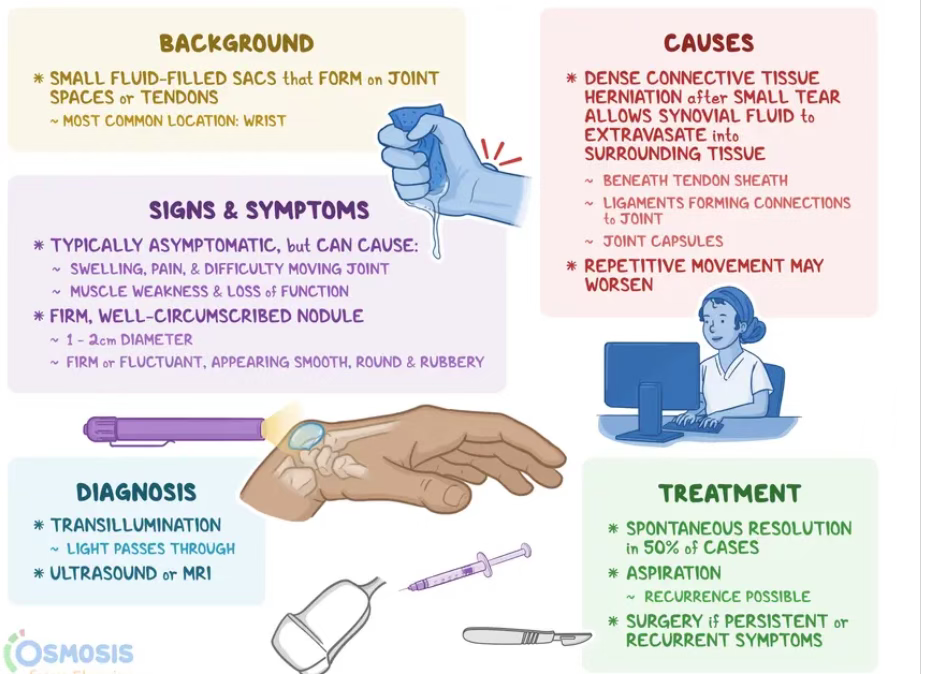
Observation and Aspiration: Gentle, Simple — But Recurrence Is Brutal
For asymptomatic cases, observation is the gold standard. Studies show 50–58% of ganglion cysts resolve spontaneously. Patient education is essential: benign, nonprogressive, and often self-limiting.
For symptomatic or cosmetic concerns, aspiration remains a popular first-line approach. It’s quick, safe, and minimally invasive — but recurrence rates reach up to 59%, with reports ranging from 7% to 72%. The variation reflects differences in aspiration completeness and technique.
Adding steroids? The data is a mess.
Two 2025 RCTs reached opposite conclusions — one favoring steroid injection over surgery, the other showing the reverse. The inconsistency and risk of skin atrophy or hypopigmentation make steroids a poor default choice.
🩺 Clinical takeaway: Aspiration is a reasonable diagnostic and temporary measure, not a cure. Always warn patients about the high chance of recurrence.
Surgical Excision: The Only Definitive Option — If Done Right
When pain, nerve compression, or recurrent cysts appear, surgical excision offers the most reliable outcome.
A 2015 meta-analysis confirmed that surgery reduces recurrence risk by 76% compared to aspiration.
- Open excision: Direct visualization, more thorough stalk removal; minor downsides are scarring and mild stiffness.
- Arthroscopic excision: Minimally invasive, faster recovery, better cosmesis, but with a steep learning curve. Recent data (2020–2022) show conflicting results — some favor arthroscopy, others open surgery — and the deciding factor is clear: surgeon experience.
💡 The best technique isn’t universal — it’s the one the surgeon performs most completely and confidently.
The priority remains: complete stalk and joint capsule removal to eliminate the one-way valve mechanism.
The Three Evidence “Traps” You Might Be Falling Into
- Trap #1 – Believing Aspiration = Cure It’s not. Aspiration decompresses but doesn’t close the joint communication — relapse is the rule, not the exception.
- Trap #2 – Overtrusting Steroid Injection Conflicting data, inconsistent effects, and real risks (atrophy, depigmentation) make steroids unreliable for ganglion cyst management.
- Trap #3 – “One Technique Fits All” Mentality Open vs arthroscopic isn’t about superiority; it’s about precision. Choose the technique that ensures full stalk excision and capsular management.
The decision pathway should remain tiered —
Observation → Aspiration (informed recurrence) → Surgery (open/arthroscopic) — always individualized to patient expectations and cyst behavior.
Volar Wrist Ganglion: High-Risk, High-Stakes
Volar wrist cysts sit dangerously close to the radial artery and palmar cutaneous branch of the median nerve — doubling both recurrence and complication rates compared to dorsal cysts.
Thus, these require microsurgical precision or an experienced hand surgeon.
Tips:
- Use magnification for dissection.
- Always identify vascular structures before excision.
- Consider ultrasound or MRI mapping for atypical or recurrent cases.
Patients must be informed that postoperative numbness, bruising, or pulsation are possible but often transient. In this region, safety > speed.
Practical Clinical Algorithm: From Clinic to OR
- Asymptomatic cyst: Observation + reassurance (self-resolution rate 50–58%).
- Mild symptoms or cosmetic concern: Aspiration — but warn of ~59% recurrence; avoid routine steroid use.
- Recurrent or painful cyst: Surgery — open or arthroscopic, chosen by surgeon expertise.
- Volar wrist cyst: Specialist-level case — microsurgical handling recommended.
The best ganglion cyst management balances invasiveness, recurrence, and patient goals — not blind adherence to a single protocol.
Authoritative Resource & Patient Education
For clear patient communication, refer to:
It concisely explains the benign nature, natural course, and treatment trade-offs — ideal for QR code linkage in clinics.
Surgeons should maintain a standardized patient handout detailing:
- Natural course and self-resolution likelihood
- Recurrence risk of aspiration
- Pros and cons of open vs arthroscopic excision
- High-risk anatomy for volar cysts
Transparency builds trust — and better postoperative satisfaction.
Disclaimer:
This article and all articles on this website are for reference only by medical professionals; specific medical problems should be treated promptly. To ensure “originality” and improve delivery efficiency, some articles on this website are AI-generated and machine-translated, which may be inappropriate or even wrong. Please refer to the original English text or leave a message if necessary. Copyright belongs to the original author. If your rights are violated, please contact the backstage to delete them. If you have any questions, please leave a message through the backstage, or leave a message below this article. Thank you!
Like and share, your hands will be left with the fragrance!
More info. https://linktr.ee/shifreeman