Introduction
Orthopedic infections and bone defects, particularly fracture-related infections (FRI), pose significant challenges in orthopedic surgery. Successful management demands a multidisciplinary approach, integrating precise diagnosis, advanced surgical techniques, antimicrobial therapy, and soft tissue reconstruction.
This article delves into current treatment options, outlining cutting-edge techniques and best practices based on the latest research. Whether you’re an orthopedic surgeon, trauma specialist, or medical researcher, this comprehensive guide provides key insights into effective bone reconstruction and infection control strategies.
What is Fracture-Related Infection (FRI)? Definition & Diagnosis
Standardized Diagnostic Criteria
FRI has gained increasing attention in orthopedic research, leading to standardized definitions and diagnostic protocols. International organizations, including the Arbeitsgemeinschaft für Osteosynthesefragen (AO) Foundation, the Orthopaedic Trauma Association (OTA), and the European Bone and Joint Infection Society (EBJIS), have developed consensus-based evidence-based diagnostic criteria [1].
Key Diagnostic Approaches:
• Clinical Evaluation: Local or systemic signs of infection.
• Imaging Techniques: Nuclear medicine imaging, CT, or MRI scans to detect osteomyelitis and implant-related infections.
• Laboratory Testing: Elevated inflammatory markers (CRP, ESR) and microbiological cultures from intraoperative samples.
• Surgical Findings: Purulent discharge, biofilm formation, or bone necrosis detected during revision surgery.
Bone Defect Treatment: Current Strategies & Innovations
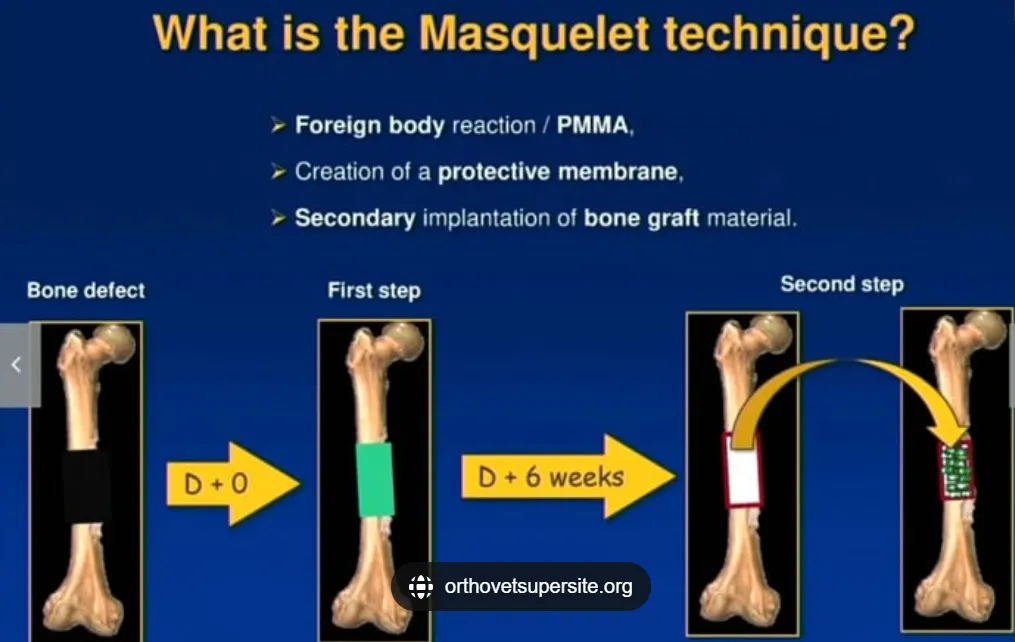
1. Induced Membrane Technique (Masquelet Procedure)
The Masquelet technique has revolutionized long-bone defect reconstruction [5,6]. It involves two surgical stages:
1️⃣ Stage One: A polymethylmethacrylate (PMMA) cement spacer is implanted into the defect site, inducing a vascularized biological membrane that promotes osteogenesis.
2️⃣ Stage Two: After 6–8 weeks, the cement is removed and replaced with autologous bone graft, leveraging the membrane’s regenerative potential.
🔹 Best suited for femoral and tibial defects.
🔹 Intramedullary nailing combined with Masquelet may outperform plate fixation [5].
🔹 Limitations: Inconsistent success rates in tibial defects due to poor vascularity.
2. Bone Transport (Ilizarov Technique)

Bone transport, facilitated by the Ilizarov circular external fixator, is a gradual distraction osteogenesis technique used to regenerate missing bone in segmental defects [7].
✅ Clears infection while simultaneously reconstructing bone.
✅ Lower failure rates in tibial and femoral nonunions compared to traditional bone grafting [8].
⚠ Challenges: High complication rates—pin tract infections, axial deviation, delayed union, or refracture [9-13].
3. Bone Grafting: Autografts & Allografts
Bone grafting remains a gold-standard technique for filling defects, categorized into:
• Autografts: Harvested from iliac crest or fibula; excellent osteogenic potential.
• Allografts: Processed cadaveric bone; structural support but lacks cellular viability [14,15].
📌 Often used in combination with antibiotic-loaded PMMA cement for infection control.
4. Vascularized Bone Grafts
For large defects (>6 cm) or poor soft tissue coverage, vascularized fibular grafting is a preferred choice [15,16].
🔹 Ensures continuous blood supply, enhancing bone healing and infection resistance.
🔹 Challenges: Requires microsurgical expertise and prolonged rehabilitation.
5. Endoprosthesis for Bone Reconstruction
For extensive bone loss due to tumors, modular endoprostheses provide an alternative to biological reconstruction [15]. However, high failure rates due to aseptic loosening remain a concern.
Managing Infection-Associated Nonunion
Infected nonunion represents one of the most difficult-to-treat orthopedic conditions. Treatment typically follows:
✅ Debridement & Implant Removal: Excision of infected bone, soft tissue, and biofilm-covered implants [17,18].
✅ Stabilization Strategy: Decision between intramedullary nailing, external fixation, or hybrid constructs.
✅ Adjunctive Therapy: Local antibiotic delivery via cement spacers or resorbable carriers.
DAIR Surgery: Debridement, Antibiotics & Implant Retention
The DAIR procedure (Debridement, Antibiotics, and Implant Retention) is a controversial approach for treating fracture-related infections (FRI) without removing stable implants [1,2].
Is DAIR Effective?
🚨 Failure Rate: 21.4% failure rate reported in multicenter trials [1,2].
🚨 Inferior Outcomes: Less successful than implant exchange or conversion to external fixation [1,2].
🚨 Best Candidates: Patients with stable implants, early-stage infection, and intact soft tissue.
Factors Affecting DAIR Success:
• Use of Local Antibiotics: Reduces reinfection rates from 18.7% to 10.0% [3].
• Soft Tissue Management: Free flap reconstruction decreases failure from 19.6% to 7.9% [5,6].
• Close Monitoring: Essential for early detection of implant loosening or skin breakdown [6].
⚠ Key Consideration: If DAIR fails, early intervention is critical to prevent progression to chronic osteomyelitis.
The Role of Antibiotics in Orthopedic Infections
📌 Local vs. Systemic Antibiotic Therapy
Local antibiotic therapy (PMMA cement, antibiotic-coated implants) achieves higher drug concentrations at the infection site while minimizing systemic toxicity [20,21].
📌 Recent Data: Studies confirm 10% lower recurrence rates with local antibiotic delivery [20].
Soft Tissue Reconstruction: Crucial for Infection Control
In severe infections with soft tissue compromise, effective soft tissue coverage is essential.
🔹 Free Flaps: Anterolateral thigh (ALT) or latissimus dorsi flaps ensure vascularized coverage [22].
🔹 Recipient Vessels: Posterior tibial artery is the most reliable lower limb option [23].
🚨 Failure to address soft tissue deficits leads to chronic osteomyelitis and implant failure.
Economic Impact of Orthopedic Infections
Beyond clinical complications, post-fracture infections impose a severe financial burden.
📉 Patients with FRI are significantly more likely to be unemployed within five years post-injury [28].
Future Directions: Where is Orthopedic Research Headed?
🔬 Optimizing DAIR Indications—better selection criteria for implant retention.
🔬 Biodegradable Antibiotic Carriers—replacing PMMA spacers to eliminate revision surgery.
🔬 Personalized Bone Regeneration Strategies—gene therapy and 3D-printed scaffolds for enhanced healing.
Conclusion: Evolving Strategies for Complex Orthopedic Infections & Bone Defects
Managing FRI and bone defects requires multifaceted approaches, from precise diagnosis to advanced reconstruction techniques. As research advances, integrating soft tissue coverage, infection control, and bone regeneration will be key to improving patient outcomes.
🔗 For in-depth guidelines, visit AO Foundation.
✅ Meta Description (SEO Optimized):
Discover the latest treatment strategies for orthopedic infections and bone defects, including DAIR surgery, Masquelet technique, bone transport, and antibiotic therapy. Learn how to optimize FRI management for better patient outcomes.
Disclaimer:
This article and all articles on this website are for reference only by medical professionals; specific medical problems should be treated promptly. To ensure “originality” and improve delivery efficiency, some articles on this website are AI-generated and machine-translated, which may be inappropriate or even wrong. Please refer to the original English text or leave a message if necessary. Copyright belongs to the original author. If your rights are violated, please contact the backstage to delete them. If you have any questions, please leave a message through the backstage, or leave a message below this article. Thank you!
Like and share, your hands will be left with the fragrance!