Meta Description:
Compare HTO vs UKA for medial knee osteoarthritis based on deformity origin, cartilage wear, age, and implant longevity. Learn how to choose the right surgical strategy with evidence-based insights.
HTO vs UKA: Why Most Surgeons Still Get This Decision Wrong
Here’s the uncomfortable truth.
Choosing between HTO vs UKA for medial knee osteoarthritis is not about preference.
It’s about precision.
Yet many decisions are still based on outdated rules:
- “Under 60 → HTO”
- “Over 60 → UKA”
That thinking is dangerous.
Because the wrong choice doesn’t just fail—it accelerates joint destruction.
The real issue? Surgeons often ignore the mechanical origin of deformity and the biological condition of cartilage.
According to the AO Foundation, alignment and load distribution are the foundation of joint preservation.
If you misread the deformity…
👉 You don’t treat the disease.
👉 You amplify it.
That’s why understanding HTO vs UKA for medial knee osteoarthritis is no longer optional—it’s critical.
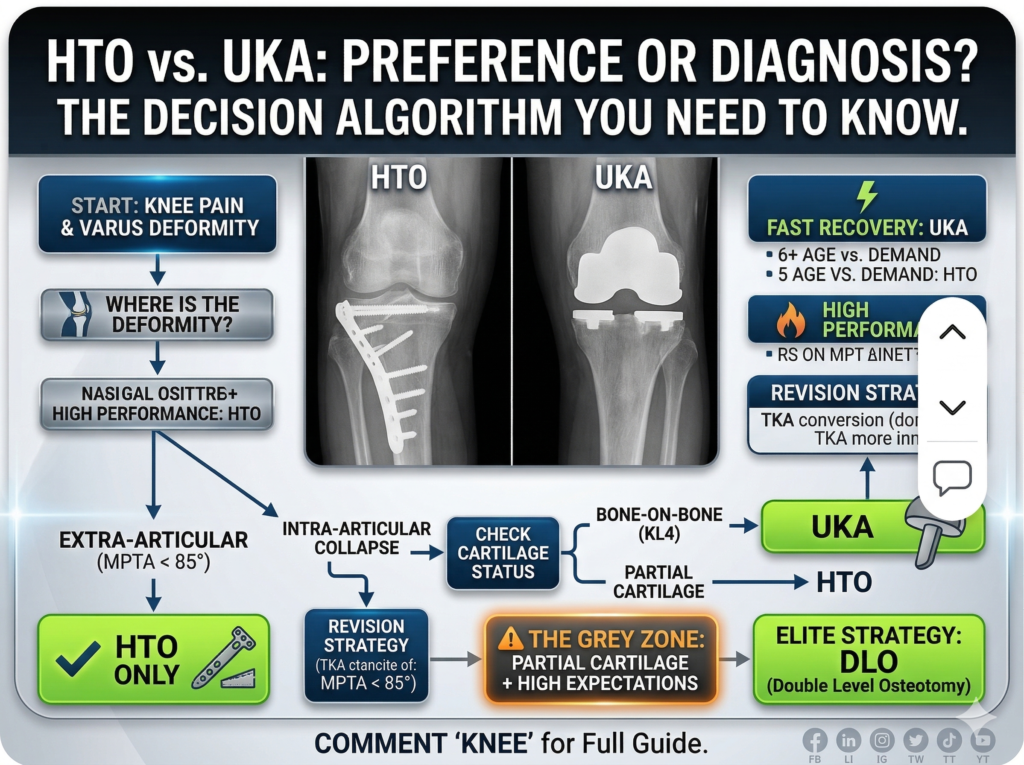
The First Rule: Identify the True Source of Deformity
Before anything else, you must answer one question:
👉 Where does the varus deformity come from?
This is the foundation of HTO vs UKA for medial knee osteoarthritis decision-making.
🔥 Extra-articular deformity → Choose HTO
- MPTA < 85°
- Tibial varus deformity present
👉 Solution: High Tibial Osteotomy (HTO)
You correct the bone.
If you choose UKA here?
You create uneven implant loading → early failure.
🔥 Intra-articular deformity → Choose UKA
- MPTA > 85°
- JLCA > 3°–5° (correctable)
- Cartilage collapse + ligament laxity
👉 Solution: Unicompartmental Knee Arthroplasty (UKA)
You restore joint space.
👉 Key insight:
HTO corrects alignment. UKA restores joint mechanics.
Confuse the two—and the outcome collapses.
Cartilage Damage: The Absolute Turning Point
If there is one factor that defines HTO vs UKA for medial knee osteoarthritis, it is this:
👉 Is it bone-on-bone?
🔴 Severe cartilage loss (Bone-on-bone)
- Ahlbäck III–IV / KL Grade 4
👉 Strongly favors UKA
Why?
Because HTO cannot rebuild cartilage effectively.
Studies show:
- HTO revision rate up to 74% at 16 years in severe cases
👉 Translation:
Wrong indication = delayed failure.
🟢 Partial cartilage loss
- Ahlbäck I–II / KL Grade 2–3
👉 Strongly favors HTO
Why?
Because cartilage still exists.
Load redistribution allows recovery.
👉 Danger of UKA here:
- Overstuffing the joint
- Accelerating lateral compartment degeneration
👉 Bottom line:
Cartilage condition is the real decision line in HTO vs UKA for medial knee osteoarthritis.
Age & Activity: The Return-to-Sport Paradox
Forget age alone.
The real question is:
👉 What life does the patient want after surgery?
⚡ UKA: Fast recovery, limited ceiling
- Rapid pain relief
- Low complication rate
- Suitable for low–moderate activity (Tegner < 5)
👉 Ideal for:
- Older patients
- Daily life priority
- No heavy labor
⚡ HTO: Slow recovery, high ceiling
- Longer rehab
- Higher early complication risk (≈5x UKA)
- Preserves natural joint
👉 Advantage:
- Return to high-impact activity (Tegner > 5)
- Better kneeling ability
👉 Ideal for:
- Younger patients
- Athletes / labor-intensive jobs
👉 Reality:
HTO vs UKA for medial knee osteoarthritis is not about age. It’s about ambition.
Implant Longevity: The Hidden Cost Nobody Talks About
This is where the decision becomes strategic.
Both HTO and UKA are not final solutions.
They are bridges to Total Knee Arthroplasty (TKA).
🔴 UKA → TKA (High-risk conversion)
- Bone loss after implant removal
- Need for:
- stems
- augments
- complex reconstruction
👉 Revision risk:
- 2.3–2.7x higher than HTO conversion
🟢 HTO → TKA (Near-primary simplicity)
- Bone stock preserved
- Standard TKA possible
👉 Outcome:
- Similar to primary TKA
👉 Conclusion:
Choosing UKA today may complicate tomorrow. Choosing HTO preserves future options.
This is a critical layer in HTO vs UKA for medial knee osteoarthritis strategy.
The 4-Step Decision Algorithm (Clinical Playbook)
Here is a simplified decision framework for HTO vs UKA for medial knee osteoarthritis:
✅ Step 1: Check ACL
- ACL deficient + slope issues → ❌ UKA
👉 Choose HTO
✅ Step 2: Pure intra-articular disease
- Bone-on-bone
- MPTA > 85°
- JLCA > 3°
👉 Choose UKA
✅ Step 3: Pure bony deformity
- MPTA < 85°
- Partial cartilage loss
👉 Choose HTO
⚠️ Step 4: Grey Zone
Mixed pathology = hardest cases.
Options:
- Low demand → UKA
- Joint preservation → HTO
- High-demand athlete → DLO (Double Level Osteotomy)
👉 Important:
Single HTO success rate for high-impact return?
<7%
DLO is the only realistic upgrade.
Final Thought: This Is Not a Choice—It’s a Strategy
The debate of HTO vs UKA for medial knee osteoarthritis is misleading.
It’s not about which is better.
It’s about:
👉 Right patient
👉 Right pathology
👉 Right timing
Make the wrong call…
And you don’t just fail the surgery.
You fail the patient’s future.
More info.