The Corona Mortis, ominously nicknamed the “Crown of Death,” is a vascular anomaly that poses significant risks in pelvic fracture surgeries. Its presence demands both anatomical awareness and precise hemorrhage control strategies to prevent life-threatening complications. This article delves into the anatomical significance, injury mechanisms, and evidence-based management techniques for this vascular variant, ensuring surgeons are prepared for its challenges.
Anatomical Definition and Clinical Relevance
What is the Corona Mortis?
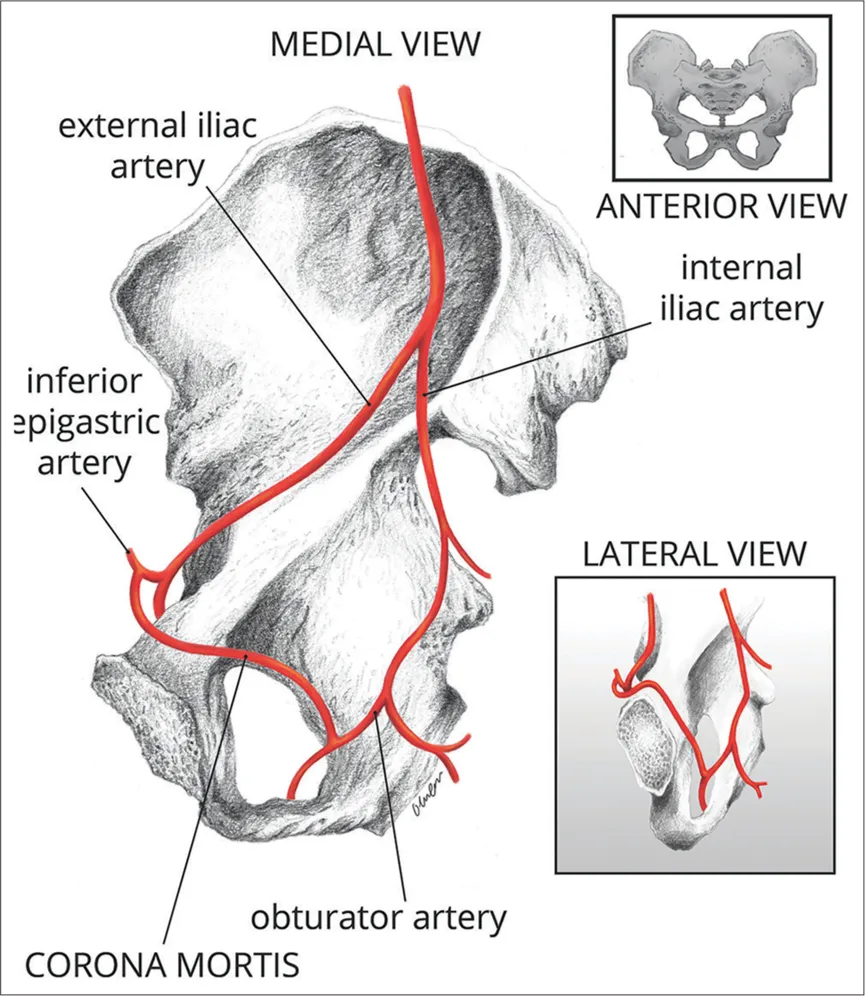
The Corona Mortis is an anastomotic connection between the obturator artery (branch of the internal iliac artery) and either the external iliac artery or its branch, the inferior epigastric artery. Found in up to one-third of clinical cases, its prevalence is even higher in cadaveric studies, reaching up to 84%. This vascular anomaly plays a critical role in collateral circulation but becomes a surgical hazard in pelvic trauma.
Key points include:
- Venous connections are more common (70%) than arterial ones.
- Gender differences exist, with females showing a higher prevalence.
- Positioned 3-7 cm from the pubic symphysis, it lies behind the superior pubic ramus, making it vulnerable during anterior pelvic surgeries.
Clinical Risks
The Corona Mortis is particularly dangerous during:
- Pelvic fractures, especially those involving the superior pubic ramus.
- Surgical procedures in the anterior pelvic ring, where its injury can cause massive hemorrhage.
Its average diameter of 2-4 mm is comparable to major vessels like the radial artery, making bleeding control both critical and challenging.
Mechanisms of Injury
Traumatic Injury
Pelvic fractures, even those considered stable, can result in Corona Mortis injury. The vessel’s location makes it susceptible to direct trauma, particularly in fractures involving the superior pubic ramus. Once injured, the vessel retracts into the pelvic cavity, leading to uncontrolled bleeding that is difficult to access.
Iatrogenic Injury
Unfamiliarity with this vascular variant increases the risk of iatrogenic injury during surgical approaches to the pelvis. Surgeons must be cautious when operating in the retropubic region, as accidental damage can lead to significant hemorrhage.
Hemorrhage Management Strategies
Endovascular Techniques
Percutaneous angiographic embolization is the gold standard for managing hemorrhage from a Corona Mortis injury. This minimally invasive technique is particularly effective in elderly or hemodynamically unstable patients.
Key steps include:
- Super-selective catheterization of the bleeding vessel.
- Embolization using materials like gel foam or micro-coils.
For example, in a case of active extravasation from the left external iliac artery, embolization successfully controlled the bleeding, stabilizing the patient.
Surgical Approaches
When embolization is unavailable or impractical, surgical techniques are essential. Recommended strategies include:
- Immediate ligation of the vessel upon identification.
- Extending the medial incision by 2-3 cm for better exposure.
- Approaches like the ilioinguinal or anterior combined endopelvic method allow direct visualization for coagulation or ligation.
In emergency settings, preperitoneal pelvic packing may serve as an alternative to control bleeding until definitive care can be provided.
Preventive Measures
Preventing Corona Mortis injury requires meticulous preoperative planning and anatomical understanding. Steps to minimize risks include:
- Angiographic mapping of the pelvis to identify the presence and location of the vessel.
- Careful subperiosteal dissection during minimally invasive procedures.
- Comprehensive training for surgeons on the anatomical variability of the Corona Mortis.
Post-Intervention Monitoring
After successful hemorrhage control, patients should be closely monitored in a high-dependency unit. Key post-operative measures include:
- Serial hemoglobin checks to detect ongoing blood loss.
- Follow-up imaging, such as contrast-enhanced CT or repeat angiography, to confirm the absence of further extravasation.
- Gradual mobilization, particularly in elderly patients, to prevent complications like deep vein thrombosis.
Case Studies: Lessons from the Field
Traumatic Rupture
A 41-year-old male with an open-book pelvic fracture presented with hemodynamic instability. Despite no initial signs of active bleeding on CT angiography, conventional angiography later revealed active extravasation from both the left obturator artery and a Corona Mortis. Super-selective embolization successfully controlled the hemorrhage.
Low-Energy Trauma
A 61-year-old female sustained a stable pelvic fracture from a low-energy fall. Unexpectedly, she developed significant bleeding from the Corona Mortis, requiring embolization. Post-intervention, her fracture was managed conservatively, and she gradually regained mobility.
Conclusion
The Corona Mortis represents a critical vascular challenge in pelvic surgery and trauma care. Its anatomical variability and potential for life-threatening hemorrhage demand heightened awareness and preparedness. By combining preventive measures, advanced endovascular techniques, and precise surgical interventions, surgeons can effectively manage this formidable vascular anomaly.
Disclaimer:
This article and all articles on this website are for reference only by medical professionals; specific medical problems should be treated promptly. To ensure “originality” and improve delivery efficiency, some articles on this website are AI-generated and machine-translated, which may be inappropriate or even wrong. Please refer to the original English text or leave a message if necessary. Copyright belongs to the original author. If your rights are violated, please contact the backstage to delete them. If you have any questions, please leave a message through the backstage, or leave a message below this article. Thank you!
Like and share, your hands will be left with the fragrance!